Visual outcome after ND: YA Glaser posterior capsulotomy in pseudophakic patient
Abstract
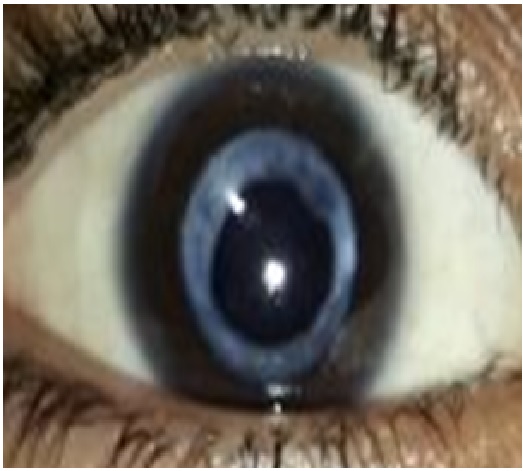
Background: Posterior capsular opacification (PCO) also called as “after cataract” is a common complication following extra capsular cataract surgery with or without posterior chamber intraocular lens implantation.An opaque membrane develops as retained cells proliferate and migrate on the posterior capsular surface.
Material and Methods: The study included a total of 100 eyes of 100 patients who were diagnosed to have posterior capsular opacification and were fulfilling all the inclusion and none of the exclusion criteria. After that they were taken for a detailed clinical examination. All patients underwent
Nd:YAG laser capsulotomy and were followed up at 1 week, 1 month and at 3 months. At every follow-up detailed examination was done. BCVA and any complications were noted.
Results:Of the 100 patients, 45 (45%) were male and 55 (55%) were female. Majority of the patients were in the age group 61-70 years. The average time interval between cataract surgery and Nd-YAG laser capsulotomy was between 2-4 years. In the type of PCO seen,84 (84.0%) patients were having Elsching pearls type of PCO, 8 (8.0%) patients were having fibrous type of PCO and 8 (8.0%) patients were having Sommering ring type of PCO. The pre laser visual acuityin more than 62% of eyes was 6/60 to FC while 38% had visual acuity of 6/36 to 6/18. Visual acuity of 6/18 or better was achieved in 27% of eyes while 73% recovered to 6/12 to 6/6. None of these eyes showed further deterioration in visual acuity. The highest energy requirement was in the Fibrous PCO s0.89 ± 0.15 J, followed by Sommering Ring PCO 0.70 ± 0.17 J and least energy was in Elsching pearls 0.47 ± 0.24 J. The comparison of mean energy between the type of PCO was found to be statistically significant (P<0.05), showing that the mean energy was varying between the types of PCO.
Conclusion: Neodymium-YAG capsulotomy for PCO is rewarding procedure inadults and has good visual outcome.
Downloads
References
2. Keeffe J, Taylor HR, Fotis K, Pesudovs K, Flaxman SR, Jonas JB, Leasher J, Naidoo K, Price H, White RA, Wong TY, Resnikoff S, Bourne RR, Vision Loss Expert Group of the Global Burden of Disease Study Prevalence and causes of vision loss in Southeast Asia and Oceania: 1990-2010. Br J Ophthalmol. 2014; 95(8):586–591.doi: 10.1136/bjophthalmol-2013-304050.[pubmed]
3. Apple DJ, Peng Q, Visessook N, et al. Eradication of posterior capsule opacification: documentation of a marked decrease in Nd:YAG laser posterior capsulotomy rates noted in an analysis of 5416 pseudophakic human eyes obtained postmortem. Ophthalmology. 2001 Mar;108(3):505-18.[pubmed]
4. Hasan KS, Adhi MI, Aziz M, et al. Nd:YAG laser posterior capsulotomy. Pak Ophthalmol. 1996; 12: 3-7.
5. Kundi NK, Younas M. Nd-YAG Laser posterior capsulotomy. J Med Sciences. 1998; 8: 90-4.
6. Emery J. Capsular opacification after cataract surgery. CurrOpinOphthalmol. 1999 Feb;10(1):73-80.[pubmed]
7. Bilal Bashir et al. Visual outcome after Nd: Yag Laser Anterior Capsulotomy in Patients with Anterior Capsular Contraction Syndrome. Ophthalmology Update Vol. 12. No. 4, October-December 2014
8. Mohammad Younas Khan et al. Visual Outcome after Nd-YAG Capsulotomy in Posterior Capsule Opacification. Pak J Ophthalmol 2006, Vol. 22 No.2
9. Gopinath GS, Satish K, Srivastava N, Patil S, Afshan R. Visual Outcome and Complications of YAG Laser Therapy for Posterior Capsular Opacification Following Cataract Surgery. Int J Sci Stud 2015;3(3):65-68.
10. Pankaj Soni et al. Nd-YAG laser posterior capsulotomy and visual outcome. Indian Journal of Clinical and Experimental Ophthalmology, July-September,2016;2(3): 271-27
Copyright (c) 2018 Author (s). Published by Siddharth Health Research and Social Welfare Society

This work is licensed under a Creative Commons Attribution 4.0 International License.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative



















 Therapoid
Therapoid

