Comparison of conjunctival free autograft and Rotational flap technique in primary pterygium surgery: Visual changes and safety profiles
Abstract
Aims and objectives: To evaluate the postoperative symptomatic comfort, visual changes, complication and rate of recurrence in free conjunctival autograft and rotational flap technique in primary pterygium surgery.
Materials & Methods: This prospective study was conducted in 60 eyes of 60 patients, presented with primary progressive nasal pterygium larger than 1mm causing symptomatic discomfort, astigmatism and cosmetic disfigurement. Patients were divided into two groups randomly. In group A, patients with pterygium excision with free conjunctival autograft and group B, pterygium excision with rotation flap technique were included. Post-operative day 1 symptomatic comfort (symptoms and signs), graft stability, corneal clarity and any complication were noted. Visual acuity (VA), auto-refracto keratometer measurements and detailed biomicroscopic examinations, were performed preoperatively and postoperatively at 1month and 3 months.
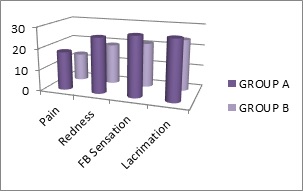
Results: Most of the patients in our study were in the middle age group of 40-49 years (41.6%). Out of 60 patients, 35 were males (58.4%) and 25 were females (41.6%). Patients with outdoor activities had a higher prevalence of pterygium (78.4%). The incidence of pterygium was more in the right eye (60%) than left eye (40%). Of the 60 patients, Grade I, II and III pterygium was 20%, 56.7% and 23.3% in group A and 16.7%, 63.3% and 20% in group B respectively. The mean symptomatic score was statistically significantly higher for group A for each factor (P<0.05). In the 3rd month, the overall patient’s satisfaction score was significantly higher in group B (P<0.05).
Conclusion: Both surgical techniques were equally effective in terms of visual acuity, astigmatism and recurrence. The patient’s satisfaction score was significantly higher in the rotation flap technique group.
Downloads
References
Di Girolamo N, Chui J, Coroneo MT, Wakefield D. Pathogenesis of pterygia: role of cytokines, growth factors, and matrix metalloproteinases. Prog Retin Eye Res. 2004 Mar;23(2):195-228. doi: 10.1016/j.preteyeres.2004.02.002.
Coroneo MT, Di Girolamo N, Wakefield D. The pathogenesis of pterygia. Curr Opin Ophthalmol. 1999 Aug;10(4):282-8. doi: 10.1097/00055735-199908000-00011.
Di Girolamo N, Coroneo MT, Wakefield D. UVB-elicited induction of MMP-1 expression in human ocular surface epithelial cells is mediated through the ERK1/2 MAPK-dependent pathway. Invest Ophthalmol Vis Sci. 2003 Nov;44(11):4705-14. doi: 10.1167/iovs.03-0356.
Golu A, Gheorghişor I, Bălăşoiu AT, Baltă F, Osiac E, Mogoantă L, Bold A. The effect of ultraviolet radiation on the cornea - experimental study. Rom J Morphol Embryol. 2013;54(4):1115-20.
Riordan-Eva P, Kielhorn I, Ficker LA, Steele AD, Kirkness CM. Conjunctival autografting in the surgical management of pterygium. Eye (Lond). 1993;7 ( Pt 5):634-8. doi: 10.1038/eye.1993.146.
Alpay A, Uğurbaş SH, Erdoğan B. Comparing techniques for pterygium surgery. Clin Ophthalmol. 2009;3:69-74. Epub 2009 Jun 2. PMID: 19668546; PMCID: PMC2709008.
Narsani AK, Nagdev PR, Memon MN. Outcome of recurrent pterygium with intraoperative 0.02% mitomycin C and free flap limbal conjunctival autograft. J Coll Physicians Surg Pak. 2013 Mar;23(3):199-202.
Rubinfeld RS, Pfister RR, Stein RM, Foster CS, Martin NF, Stoleru S. et al. Serious complications of topical mitomycin-C after pterygium surgery. Ophthalmology. 1992 Nov;99(11):1647-54. doi: 10.1016/s0161-6420(92)31749-x.
Safianik B, Ben-Zion I, Garzozi HJ. Serious corneoscleral complications after pterygium excision with mitomycin C. Br J Ophthalmol. 2002 Mar;86(3):357-8. doi: 10.1136/bjo.86.3.357.
Mahdy MA, Bhatia J. Treatment of primary pterygium: Role of limbal stem cells and conjunctival autograft transplantation. Oman J Ophthalmol. 2009 Jan;2(1):23-6. doi: 10.4103/0974-620X.48418.
Koranyi G, Seregard S, Kopp ED. The cut-and-paste method for primary pterygium surgery: long-term follow-up. Acta Ophthalmol Scand. 2005 Jun;83(3):298-301. doi: 10.1111/j.1600-0420.2005.00465.x.
Aslan L, Aslankurt M, Aksoy A, Ozdemir M, Yüksel E. Comparison of wide conjunctival flap and conjunctival autografting techniques in pterygium surgery. J Ophthalmol. 2013;2013:209401. doi: 10.1155/2013/209401.
Maheshwari S. Effect of pterygium excision on pterygium induced astigmatism. Indian J Ophthalmol. 2003 Jun;51(2):187-8.
Mohite, U. S., N. B. Dole, and S. S. Jadhav. "Effectiveness of pterygium surgery on corneal astigmatism." Med Pulse Int J Ophthalmol 3 (2017): 12-17.
Avisar R, Mekler S, Savir H. [Effect of pterygium excision on keratometric readings]. Harefuah. 1994 Jan 16;126(2):63-5, 112, 111. Hebrew.
Lindsay RG, Sullivan L. Pterygium-induced corneal astigmatism. Clin Exp Optom. 2001 Jul;84(4):200-203. doi: 10.1111/j.1444-0938.2001.tb05026.x.
Ti SE, Chee SP, Dear KB, Tan DT. Analysis of variation in success rates in conjunctival autografting for primary and recurrent pterygium. Br J Ophthalmol. 2000 Apr;84(4):385-9. doi: 10.1136/bjo.84.4.385.
Copyright (c) 2021 Author (s). Published by Siddharth Health Research and Social Welfare Society

This work is licensed under a Creative Commons Attribution 4.0 International License.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative



















 Therapoid
Therapoid

