Incidence of retinopathy of prematurity in neonatal intensive care unit in a tertiary care centre in central India
Abstract
Introduction: Retinopathy of Prematurity (ROP) is one of the most common disorders affecting the eyes of premature infants, characterized by abnormal proliferation of retinal blood vessels. In the absence of treatment, it can result in retinal detachment and permanent loss of vision. Advances in neonatal care have resulted in increase in survival rates of very premature infants and consequent increase in incidence of ROP.
Purpose: The present study, conducted in a single NICU in a tertiary care centre, estimates the incidence of ROP and evaluates the associated risk factors.
Materials and Methods: A retrospective cohort study was performed on premature infants in a tertiary care unit in Central India between February 2018 to July 2019. One hundred and four infants were included in the study based on the following inclusion criteria: Gestational age below 34 weeks, Birth weight below 1700 gms, or babies born with gestational age above 34 weeks or birth weight above 1700 gms, but with any of the following: respiratory distress syndrome, sepsis, intraventricular hemorrhage, blood transfusions or multiple gestation. Follow up was done until disease resolution or until treatment criteria were achieved.
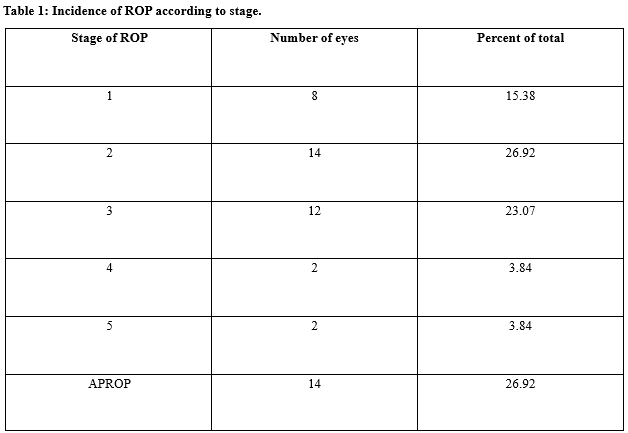
Results: A total of 104 infants were evaluated after applying the inclusion criteria. Babies that were screened had mean GA of 30.28 weeks (SD: 2.84, range: 26–36 weeks). Babies with ROP had a mean GA of 28.91 weeks (range: 26–36 weeks, SD: 2.64). The mean Birth weight for the cohort was 1468 g (standard deviation [SD]: 300, range: 830–1870 g). Babies in ROP group had a mean BW of 1278 g (SD: 0.27, range: 830 –1726 g). The incidence of ROP of any stage was found to be 25.96%. Babies with a GA of <28 weeks had the highest incidence of ROP (62.8%). A significant association was noted between ROP and oxygen therapy(P<0.01) as well as RDS(P<0.02).
Conclusion: This study found incidence of ROP to be 25.96% in the target population and showed respiratory distress and Oxygen therapy to be significant risk factors associated with the disease.
Downloads
References
Blencowe H, Lawn JE, Vazquez T, Fielder A, Gilbert C. Preterm-associated visual impairment and estimates of retinopathy of prematurity at regional and global levels for 2010. Pediatr Res. 2013;74(1):35-49. doi: https://dx.doi.org/10.1038%2Fpr.2013.205.
Good WV, Hardy RJ, Dobson V, Palmer EA, Phelps DL, Quintos M, et al. The incidence and course of retinopathy of prematurity: Findings from the early treatment for retinopathy of prematurity study. Pediatrics. 2005;116(1):15-23. doi: https://doi.org/10.1542/peds.2004-1413.
Zin A, Gole GA. Retinopathy of prematurity-incidence today. Clin Perinatol. 2013;40(2):185-200. doi: https://dx.doi.org/10.1016/j.clp.2013.02.001.
Karna P, Muttineni J, Angell L, Karmaus W. Retinopathy of prematurity and risk factors: A prospective cohort study. BMC Pediatr. 2005;5(1):18. doi: https://doi.org/10.1186/1471-2431-5-18.
Palmer EA, Flynn JT, Hardy RJ, Phelps DL, Phillips CL, Schaffer DB, et al. Incidence and early course of retinopathy of prematurity. The cryotherapy for retinopathy of prematurity cooperative group. Ophthalmol. 1991;98(11):1628-1640. doi: https://doi.org/10.1016/s0161-6420(91)32074-8.
Azad R. Prevention of blindness due to retinopathy of prematurity: A national movement. Indian J Pediatr. 2014;81(12):1373-1375. doi: https://doi.org/10.1007/s12098-014-1411-x.
Puri S, Sarpal S, Ashat M. Screening of retinopathy of prematurity: A neglected public health issue. Ann Med Health Sci Res. 2014;4(1):S65-S66. doi: https://dx.doi.org/10.4103%2F2141-9248.131726.
International Committee for the Classification of Retinopathy of Prematurity. The international classification of retinopathy of prematurity revisited. Arch Ophthalmol. 2005;123(7):991-999. doi: https://doi.org/10.1001/archopht.123.7.991.
Section on Ophthalmology, American Academy of Pediatrics, American Academy of Ophthalmologists, American Association for Pediatric Ophthalmology and Strabismus. Screening examinations for premature infants for retinopathy of prematurity. Pediatri. 2006;117(2):572-576. doi: https://doi.org/10.1542/peds.2005-2749.
Chen J, Stahl A, Hellstrom A, Smith LE. Current update on retinopathy of prematurity: Screening and treatment. Curr Opin Pediatr. 2011;23(2):173-178. doi: https://doi.org/10.1097/MOP.0b013e3283423f35.
Murthy KR, Murthy PR, Shah DA, Nandan MR, Niranjan HS, Benakappa N. Comparison of profile of retinopathy of prematurity in semiurban/rural and urban NICUs in Karnataka, India. Br J Ophthalmol. 2013;97(6):687-689. doi: https://doi.org/10.1136/bjophthalmol-2012-302801.
Murthy KR, Babu K, Benakappa N, Murthy PR, Nagendra Niranjan. Analysis of risk factors for the development of retinopathy of prematurity in preterm infants at a tertiary referral hospital in South India. Acta Med Litu. 2006;13(3):147-151.
Chaudhari S, Patwardhan V, Vaidya U, Kadam S, Kamat A. Retinopathy of prematurity in a tertiary care center – Incidence, risk factors and outcome. Indian Pediatr. 2009;46(3):219-224.
Ashok KM, Rajalakshmi AR, Gunasekaran D, Sreeraaganidhi A study of risk factors for retinopathy of prematurity in a medical college hospital in South India to evaluate the criteria for screening for retinopathy of prematurity. J Curr Trends Clin Med Lab Biochem. 2014;2(2):31-36
Charan R, Dogra MR, Gupta A, Narang A. Incidence of retinopathy of prematurity in a neonatal care unit. Indian J Ophthalmol. 1995;43(3):123-126.
Fortes Filho JB, Eckert GU, Valiatti FB, Dos Santos PG, da Costa MC, Procianoy RS, et al. The influence of
gestational age on the dynamic behavior of other risk factors associated with retinopathy of prematurity (ROP) Graefes Arch Clin Exp Ophthalmol. 2010;248(6):893-900. doi: https://dx.doi.org/10.1007%2Fs00417-009-1248-6.
McColm JR, Fleck BW. Retinopathy of prematurity: Causation. Semin Neonatol. 2001;6(6):453-460. https://doi.org/10.1053/siny.2001.0079.
Hungi B, Vinekar A, Datti N, Kariyappa P, Braganza S, Chinnaiah S, et al. Retinopathy of prematurity in a rural Neonatal Intensive Care Unit in South India – A prospective study. Indian J Pediatr. 2012;79(7):911-915. doi: https://doi.org/10.1007/s12098-012-0707-y.
Fortes Filho JB, Eckert GU, Procianoy L, Barros CK, Procianoy RS. Incidence and risk factors for retinopathy of prematurity in very low and in extremely low birth weight infants in a unit-based approach in Southern Brazil. Eye (Lond) 2009;23(1):25-30. doi: https://doi.org/10.1038/sj.eye.6702924.
Kapoor R, Talwar R, Sachdeva S, Paul P, Yadav R, Sachdeva S. Retinopathy of prematurity in babies weighing <1800 g; with special reference to babies weighing between 1501 and 1800 g: An experience from a tertiary care hospital in Delhi. Int J Med Public Health. 2014;4(4):359-363. doi: http://dx.doi.org/10.4103/2230-8598.144066.
Shah PK, Narendran V, Kalpana N, Gilbert C. Severe retinopathy of prematurity in big babies in India: History repeating itself? Indian J Pediatr. 2009;76(8):801-804. doi: https://doi.org/10.1007/s12098-009-0175-1.
Jalali S, Matalia J, Hussain A, Anand R. Modification of screening criteria for retinopathy of prematurity in India and other middle-income countries. Am J Ophthalmol. 2006;141(5):966-968. doi: https://doi.org/10.1016/j.ajo.2005.12.016.
Wu WC, Ong FS, Kuo JZ, Lai CC, Wang NC, Chen KJ, et al. Retinopathy of prematurity and maternal age. Retina. 2010;30(2):327-331. doi: https://doi.org/10.1097/IAE.0b013e3181ba246f.
Uchida A, Miwa M, Shinoda H, Koto T, Nagai N, Mochimaru H, et al. Association of maternal age to development and progression of retinopathy of prematurity in infants of gestational age under 33 weeks. J Ophthalmol. 2014;2014:187929. doi: https://doi.org/10.1155/2014/187929.
Bizzarro MJ, Li FY, Katz K, Shabanova V, Ehrenkranz RA, Bhandari V, et al. Temporal quantification of oxygen saturation ranges: An effort to reduce hyperoxia in the Neonatal Intensive Care Unit. J Perinatol. 2014;34(1):33-38. doi: https://doi.org/10.1038/jp.2013.122.


 OAI - Open Archives Initiative
OAI - Open Archives Initiative



















 Therapoid
Therapoid

