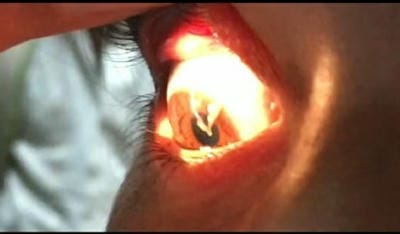
Wriggly creatures coming out of eye: case report on human ocular thelaziasis
Tripathi A.1*, Bhalla S.2
DOI: https://doi.org/10.17511/jooo.2020.i08.05
1* Anchal Tripathi, Senior Resident, Department of Ophthalmology, LLRH, GSVM Medical College, Kanpur, Uttar Pradesh, India.
2 Sonali Bhalla, Assistant Professor, Department of Ophthalmology, LLRH, GSVM Medical College, Kanpur, Uttar Pradesh, India.
Ocular Thelaziasis is an arthropod-borne, zoonotic disease of the eye affecting the conjunctival sac, lacrimal duct, and lacrimal gland caused by a nematode of the genus Thelazia. Thelazia species are transmitted by different species of Muscidae, which are a family of flies with worldwide distribution. The present study reports a case of human ocular Thelaziasis in a 13-year-old female patient. Species Thelazia callipaeda was confirmed based on microbiological examination. The patient was treated with anti-helminthic drugs and was relieved of the symptoms without recurrence.
Keywords: Thelazia callipaeda, Thelaziasis, Zoonotic disease
| Corresponding Author | How to Cite this Article | To Browse |
|---|---|---|
| , Senior Resident, Department of Ophthalmology, LLRH, GSVM Medical College, Kanpur, Uttar Pradesh, India. Email: |
Tripathi A, Bhalla S. Wriggly creatures coming out of eye: case report on human ocular thelaziasis. Trop J Ophthalmol Otolaryngol. 2020;5(8):250-253. Available From https://opthalmology.medresearch.in/index.php/jooo/article/view/172 |


 ©
©